Diagnostic Equipment
Equipment available in our State-of-the-Art EYE PRO Studio Oculistico in Torino
Computerized Vision Measurement
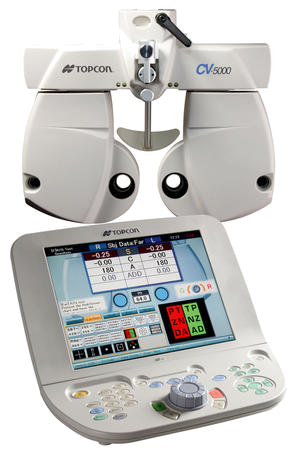
The Automated Phoropter receives the eye data obtained by the Auto-Refractometer and the glasses readings coming from the Lensmeter and applies either measurment to the embedded lenses. The lenses are then changed by the operator via the controls on the console. This system makes it very easy for the patient to appreciate the differences in vision between the old glasses prescription and the new refraction. It also supports cross cylinders for extremly precise fine tuning of the final astigmatism axis and power.
No-touch eye pressure Measurement
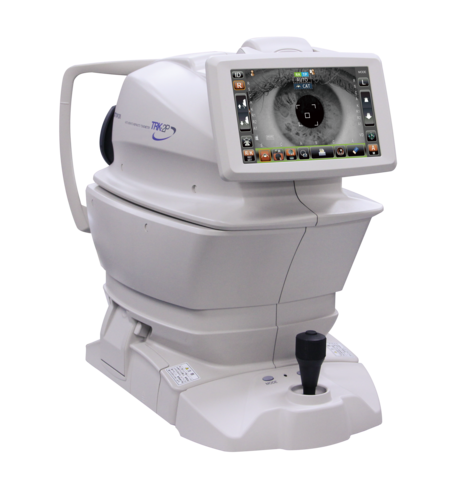
For all non glaucoma patients and thos who do not require Goldman applanation tonometry, eye pressure measurement is easily done by means of air puff tonometry. This latest device simultaneously measures central corneal thickness and shows the adjusted IOP measurement taking this important parameter into account. This is very important not to be mislead that the eye pressure is low when for example the measurement is done on an eye with very thin cornea, and viceversa. It’s especially important in post LASIK/PRK patients.
Auto Refractometer
The Auto Refractor takes an objective measurement of the refractive status of the patient’s eye. This objective measurement is the starting point for the refraction that follows, which can be done either via the traditional lens frame and the individual lenses, or via the Automated Phoropter like in our clinic.

Corneal Topography / Aberrometry
Corneal Topography is an extremely important test used to evaluate corneal astigmatism. It determines the magnitude (in diopters, D) and the axis (in degrees) of the astigmatism. With corneal topography we can identify irregular versus regular astigmatism (which is extremely important in ruling out and following up keratoconus - a serious degenerative condition of the cornea). Corneal topography is also an essential tool in evaluating the suitability for laser refractive surgery, as it can measure the central corneal thickness and identify poor candiates with weak corneas. In our center we are using the Oculus Pentacam, the most advanced corneal topographer on the market. This device also determines corneal aberrations and it is useful in planning toric IOL implantation for cataract surgery and intracorneal rings implantation for keratoconus.

Corneal Specular Microscopy
This device is used by anterior segment and corneal specialists to assess the health of the corneal endothelium (a very thin layer that lines up the internal part of the cornea and is made of many cells shaped like little hexagons). A weak endothelium can make the eye unsuitable for ICL implantation (used for high myopia) or for other intraocular surgeries. If the endothelium become too damaged it causes the cornea to swell and become cloudy, which may require corneal transplantion, either as a lamella (DSEK, DMEK) or as a full thickness graft (PK). This tool is essential in the evaluation and follow up of corneal transplants.
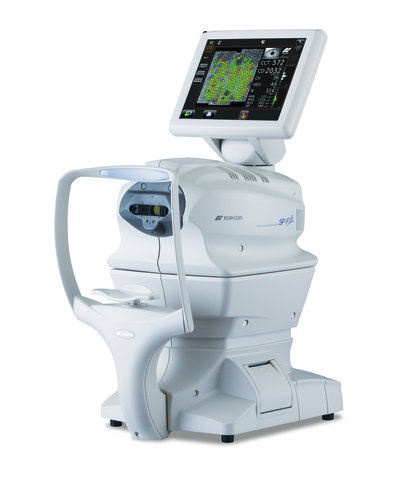
Optical Biometry (laser PCI)
Biometry is the technique of measuring the length of the eye and the curvature of the cornea, along with other internal parameters, for the purpose of calculating the correct intraocular lens (IOL) power to be implanted in the patient’s eye during cataract surgery to correct the vision. If no lens is impanted, normally it is not possible to see, since the cataract itself is a lens of a certain power which gets coudy and is removed. Until not too long ago these measurments were done with the ultrasound machine, but nowadays we use an extremely precise laser device. This technology has dramatically increased the accuracy in achieving the desired refractive outcome compared to ultrasound, with fewer eyes requiring to wear glasses for distance vision following surgery.
Dr Borasio is an internationally renowned expert in complex biometry, especially in those difficult cases following lasik or laser refractive surgery (read more).
High Resolution
Slit Lamp Photography
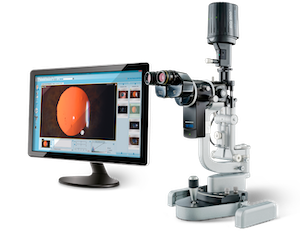
When an ocular lesion is identified during examination, we document it by means of digital photos. This allows direct and accurate comparison of the lesion size and appearance from one visit to the other. We are using the very top-of-the-range Haag Streit microscope with a professional-level digital acquisition systems to take the very best digital photos. Most centers use cheap devices such as digital cameras or iPhones attached to the optics of the slit lamp microscope.
High Resolution Ultra Wide Field
Retinal Photography
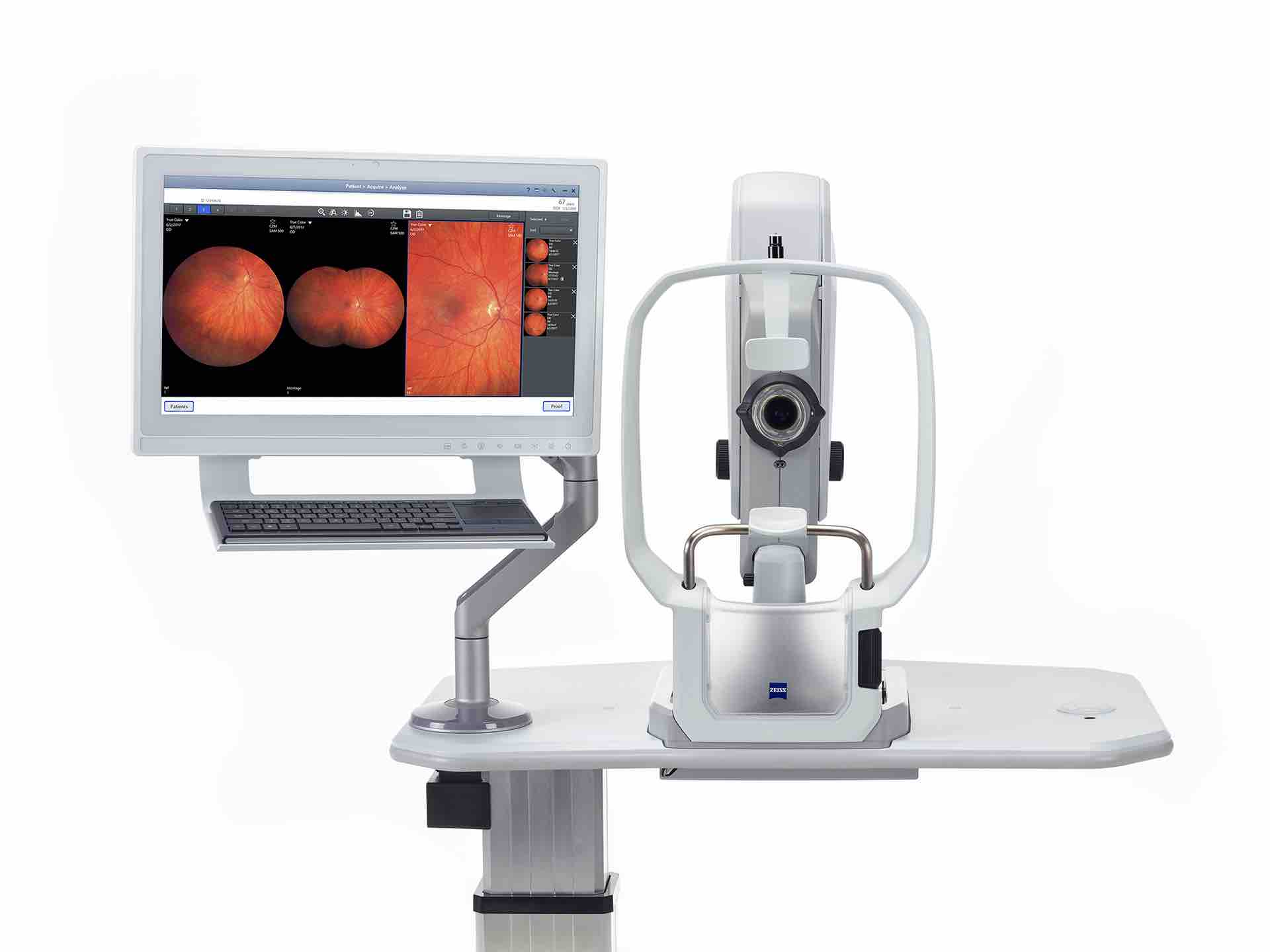
Documenting the size and shape of retinal lesions (such as vascular pathologies, optic disc alterations, retinal breaks, choroidal nevi, etc) is extremely important in the evaluation of the health of the eye. We are proud to be the first and only center in Piemonte having the revolutionary Zeiss Clarus 500, which takes extremely high resolution and ultra wide field retinal photos without having to dilate the patient's pupils.
With pupil dilation the field of view is even larger but this is not always needed. Without pupil dilation patients can drive home immediately after the consulation rather than having to wait for several hours for the drops effect to wear off.
Swept Source OCT
Retina, Glaucoma, Cornea, Angio
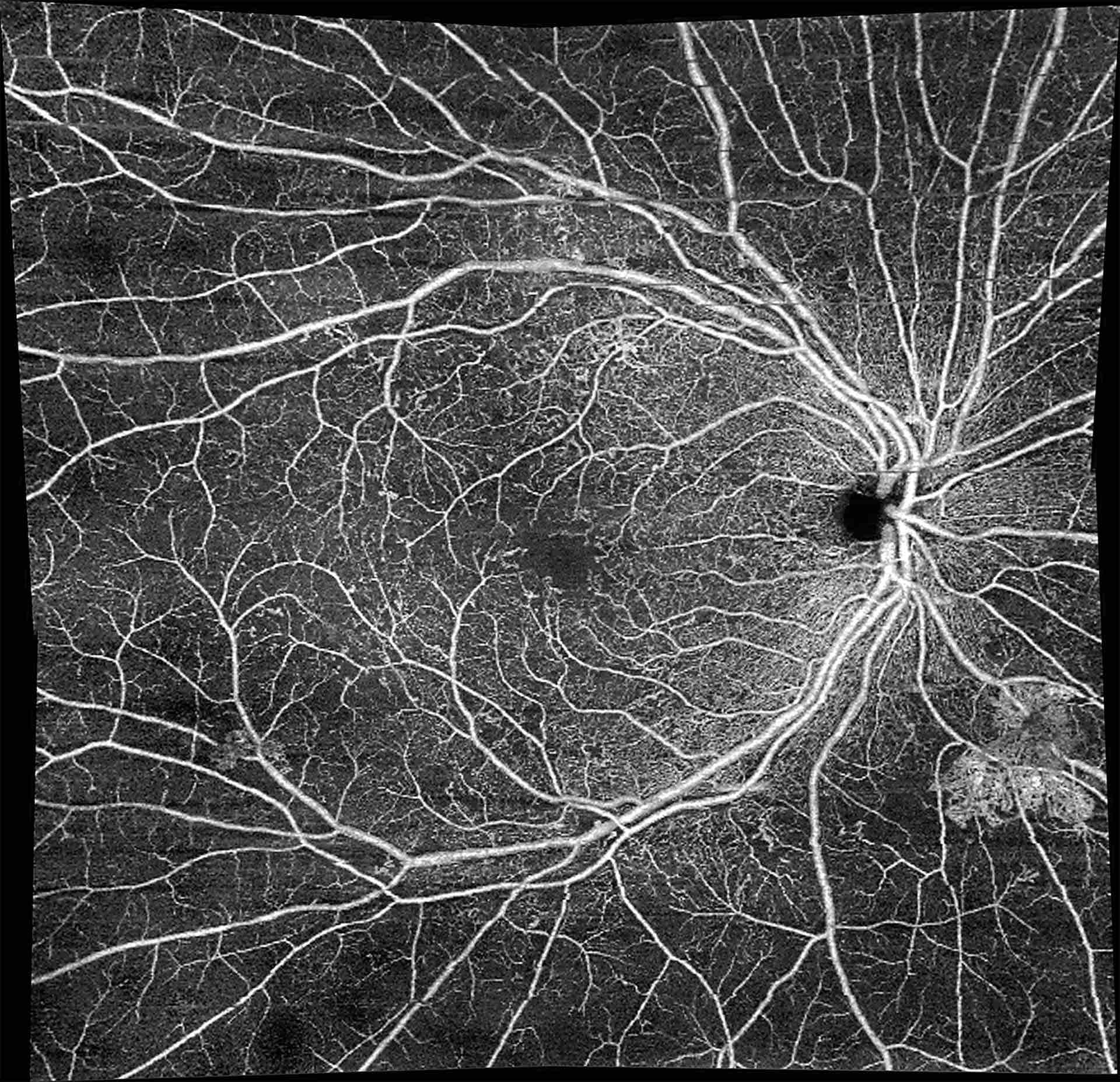
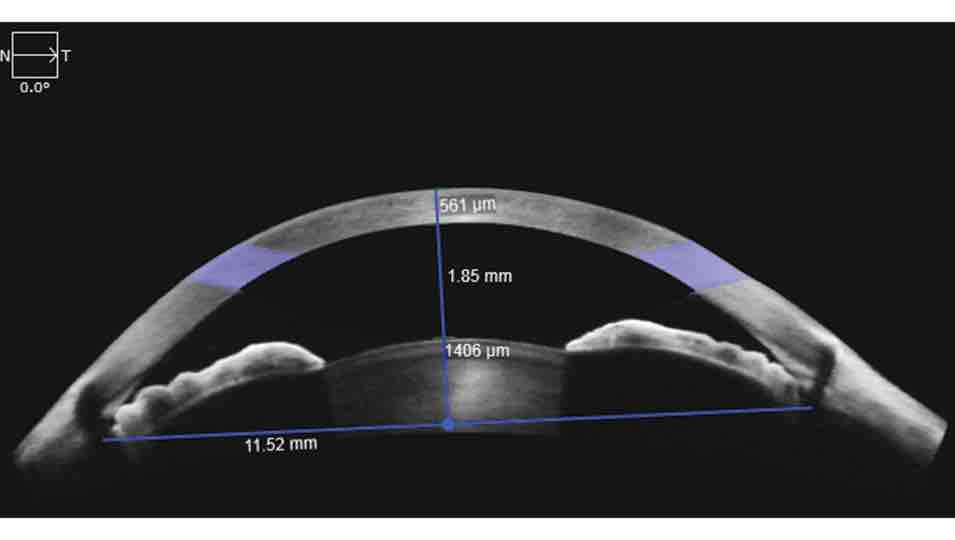
Optical Coherence Tomomography is an imaging technique that uses low-coherence infrared light to capture micrometer-resolution, two- and three-dimensional images of different structures of the eye such as the retina. The technology evolved so much to the point that now it is even able to visualize blood flow in the retinal vessels. This technique is called Angio OCT and it has several advantages compared to traditional Fluorescein Angiography. In particular it does not require the injection of contrast medium, so no longer need of the test being performed in a hospital setting since there is no longer the risk of anaphylactic shock.
The latest OCTs can also scan the anterior chamber angles (useful in narrow angle glaucoma) and the cornea (useful in determining the depth of corneal scars, LASIK flap or SMILE interface irregularities.
Visual Field Evaluation
Certain pathologies cause an alteration of the visual field. For example, in glaucoma and retinitis pigmentosa there is a restriction of the peripheral visual field. In other conditions such as papilledema there is an enlargement of the physiological paracental blind spot. In some neurological conditions there can be the loss of one half or a sector of the visual field in both eyes. Some other pathologies like cataract may cause a generalized reduction of the sensitivity to the light in all sectors. An adequate visual field is also an important requirement for driving. With this device we can identify the visual field defects and montior their changes accurately over time.
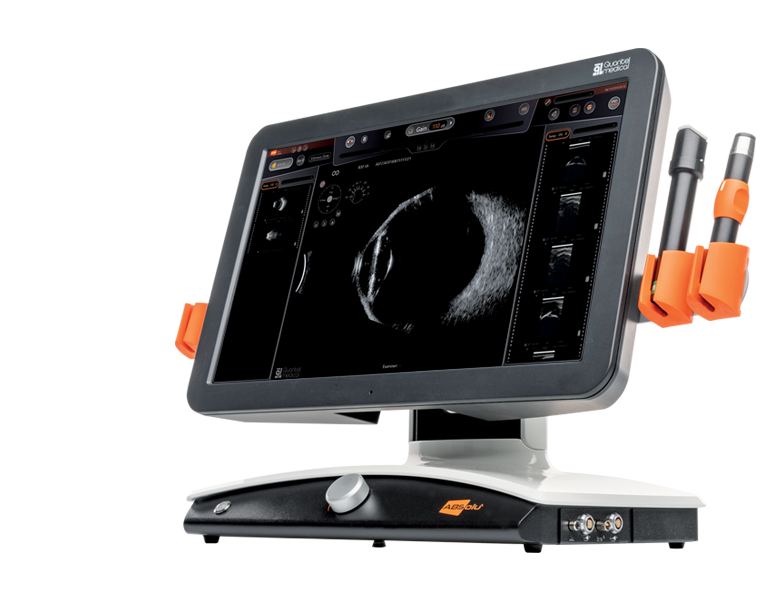
Ocular Ultrasound (A-B scan)
B-scan Ultrasound is an essential tool used to rule out the presence of retinal detachment and major internal alterations in those eyes where there is an extremely dense cataract that prevents the doctor from viualising the retina directly. It is also used to evaluate vitreous floaters (dark flies floating inside the vitreous cavity) and to measure the size of lesions such as cysts of the iris, choroidal nevi or tumors and swelling or lesions of the extraocular muscles.
A-scan Ultrasound is instead used for Biometry in those unusual cases in which the cataract is so dense that it prevents measurement by means of the more precise optical biometer.
Exophthalmometry
This device measures how much the eyes are “popping out” from the orbits and it is essential in monitoring patients with hyperthiroidism / Graves or Basedow Disease, who are suffering from proptosis / exophthalmos. It is also used to measure how much an eye is sunken inside the orbit, as it could be the case following a trauma with orbital floor fracture. The graded scale allows measurements to be compared reliably between different examinations and operators.

Color Vision Assessment
Color vision deficiencies such as those on the red-green axis (color blindness) are often inherited as X-linked genetic conditions, passed from the mother to the male child, but other types of transmission exist. Rarely they can be acquired as the result of ocular or systeic pathologies. Color deficiencies can be identified and quantified by means of Ishihara pseudoisochromatic charts, which are charts made of dots of different colors inside which numbers are inscribed. People affected can sometimes avail of some improvement in color perception by wearing special prismatic glasses that separate the green and red wavelength of the spectrum.

Stereopsis Assessment
Stereopsis is the ability of perceiving the threedimensionality of objects through the use of both eyes. People with strabismus or large differences in refraction between the eyes, or lazy eye have some alterations in the stereopsis. In our center we are using polarized lenses and a polarized visual acuity screen to accurately evaluate stereopsis.

Contrast Sensitivity
Contrast sensitivity is the ability of the eye and the brain to perceive lightly colored letters or objects against a bright background. An eye with good optics (a clear cornea with low astigmatism and negligible aberrations + a clear crystalline lens with no cataract) and a good sensor (a normal retina) does not have any issue with contrast sensitivity and is able to discern very lightly colored letters. The following conditions reduce contrast sensitiviy: corneal opacities, corneal edema, status post certain lamellar or endothelial keratoplasties, high astigmatism, high corneal aberrations, cataract, macular edema, macular membranes, status post vitreo-retinal surgery or trauma, presence of multiple artificial lenses inside the eye and amblyopia. To a certain degree, also the presence of a multifocal IOL inside the eye reduces contrast sensitivity a little. This is why not everyone is a candidate for these types of lenses. During the consultation you will be told if you are a good candidate or not according to the eye parameters and your job requirements.

Visual Acuity with Glare
Certain people, such as airplane pilots or lorry drivers, require good visual function even in the presence of glare from incoming lights. In our center we have a special visual acuity system which allows us to measurement the vision also in the presence of glare.

Dr Borasio only receives at:
EYE PRO
Studio Oculistico
Via Carlo Giordana 5, Torino, Italy
Tel: +39 392 7231024
dr@edmondoborasio.com

About Dr Borasio
Curriculum VitaeFor professionals
PC Software for OphthalmologistsiOS Apps for OphthalmologistsPost LASIK Biometry ConsultationProcedures
Laser Vision CorrectionLaser Cataract SurgeryClear Lens Exchange
Presbyopia correction
Astigmatism Correction
Multifocal IOLs
ICL Phakic lens implantationKeratoconus management
Corneal Transplantation
Pterygium excision
Iris reconstruction
Intravitreal Injections (aVEGF)YAG laser capsulotomyYAG laser iridotomyYAG laser vitreolysis (floaters)SLT laser (glaucoma)Argon laser (retina)

